Heel Spurs and Plantar Fasciitis…..is there a Difference?
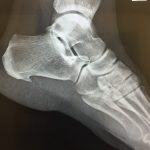
Notice the spur growing on the heel or Calcaneus
The History
You can easily see the heel spur, or as I like to call it, “Hell Spur” in the above X-ray. This patient began to experience pain in their heel region after a trail run. After an online search she diagnosed herself with Plantar Fasciitis. She diligently did all of the recommended internet home treatments. Rest, ice, Ibuprofen, stretching and rolling her foot out with a tennis ball. None of it seemed to work for her. In fact the pain seemed to be worsening. She had a Half Marathon looming and she could barely walk without a limp. She decided to come to the San Diego Running Institute for help.
There are a couple of key differences between plantar fasciitis and heel spurs. During the exam I asked a few simple questions that allowed me to immediately know that she was not dealing with traditional plantar fasciitis. Below are the differences.
- Do you have pain in your arch/heel in the morning when getting out of bed that “warms up” as you walk? If you answer yes to this question you PROBABLY have plantar fasciitis. If you answered no or yes but the pain does not warm up and actually gets worse throughout the day you PROBABLY are dealing with a heel spur.
- When you walk or run does the pain in your arch and heel seem to warm up as you go? If you answer yes you PROBABLY have plantar fasciitis. If you answer that the pain is present and actually gets worse while you walk or run than you PROBABLY have a heel spur.
- Does stretching you calf seem to help the pain in your arch/heel region? If you answer yes than you PROBABLY have plantar fasciitis. If you answer no, that stretching does not help than you PROBABLY have a heel spur.
The Exam
When a patient presents with heel and/or arch pain there are a couple of conditions we want to consider. Plantar fasciitis, plantar fasciosis, heel spur syndrome, Joggers Foot (also called a calcaneal nerve entrapment) and stress fracture of the heel. A simple orthopedic exam can quickly help eliminate a couple of these and zero in on the problem. In this case I used a flat diagnostic tool to “scrape” along the patients heel until I felt the bump that I knew was the heel spur. This finding coupled with her history allowed me to diagnose her with a heel spur and immediately begin to provide effective treatment interventions. Treatment interventions for heel spurs vary slightly from treatment interventions for plantar fasciitis. I sent the patient for an X-ray to confirm the heel spur diagnosis (see the above X-ray) and began to educate her on how to properly care for this painful condition.
The Education
Plantar Fasciitis is classified as inflammation of the plantar fascia where it originates on the heel. A heel spur is actual bone formation where the plantar fascia attaches at the heel. It is this bone formation that is painful. This is a critical point because it is not the actual spur that is painful. I have treated hundreds of patients with huge heel spurs that have no pain! You may be wondering how this can be. A good example is a patient that comes to my office with a sprained ankle. When we get the X-ray back we notice that in addition to the sprained ankle they have a huge heel spur. I will casually ask the patient “Do you have any heel pain”? The normal response is “No”, I don’t…..but years ago I did”. What this tells us is that years ago while the spur was FORMING they had heel pain. Now that the spur is done forming there is no longer pain. So it our primary goal to STOP THE SPUR FROM CONTINUING TO FORM! Once you grasp the difference and understand WHY the spur is forming fixing heel spurs becomes much easier.
So how do I Stop the Heel Spur from Forming?
My primary goals are dependent on the patient’s primary goal. If the patient has an event they are training for and want to get through that event than we use plan “A” to help ease the pain and stabilize the spur. This will minimize the formation of the heel spur. If the patient does not have a reason to train on their foot we immobilize their foot for a period of 2-6 weeks while we treat the heel spur and stop the heel spur formation in its tracks.
Plan “A” – A typical example is a runner training for a marathon, a hiker training for a trek through the mountains, a tennis player training for a big tournament or even someone whose job requires them to be on their feet and they can’t afford to rest at the current time.
- We have them immediately stop doing everything they are doing as it is obviously not working. Normal examples of things that do not work for heel spurs are icing, stretching and orthotics. It is amazing how many people are actually contributing to their pain by doing things that have been recommended by well-intentioned doctors, therapists and friends.
- We instruct them to wear whichever shoes are MOST comfortable and make their heel the happiest. For women this is often easier than men because women will often say that when they wear high heels or a wedge sandal their heel barely hurts. This makes sense because their heel is elevated transferring most of the pressure from the heel to the front of their foot.

Heels can reduce heel spur pain
- For men we can usually add a temporary heel lift into their shoes which results in a similar effect. We have a specific heel cup that we prefer that not only elevates the heel but functions as an external heel fat pad and helps cushion the painful area. It is amazing how many patients have expensive custom orthotics that are painful to them and when we replace the useless orthotics with $15 heel cups all of a sudden their heel spur pain begins to fade!

Heel lifts transfer weight off of the heel to the ball of the foot
- We instruct the person to perform self-massage using the APPROPRIATE amount of pressure. It is common for patients to tell me they are massaging their heel or arch with a golf ball or some other hard object and using entirely too much pressure which results in a bruising effect on the heel spur. Once we replace the hard object with an appropriate massage tool and use a reasonable amount of pressure the results change from bad to good immediately.

Heel cups provide cushion and transfer weight off the Heel Spur
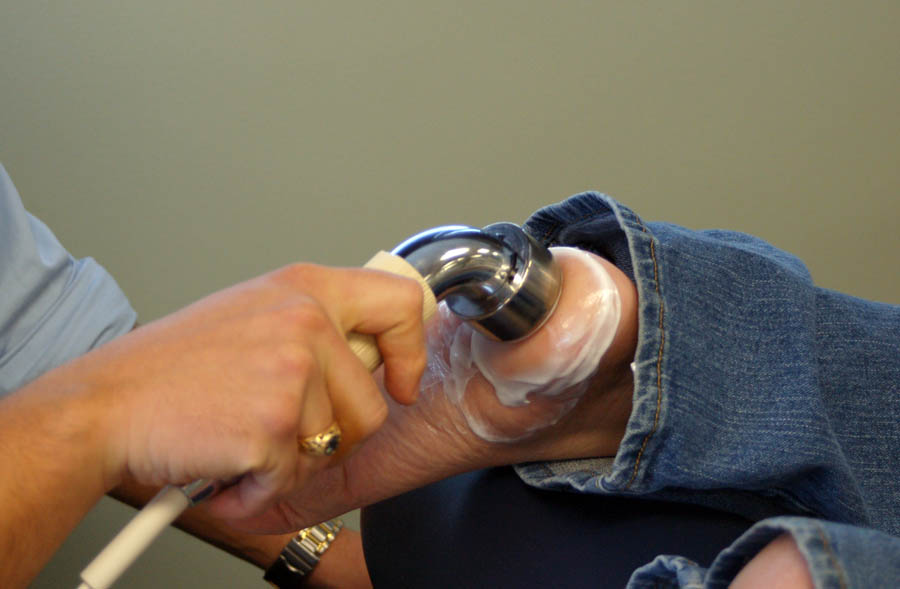
- We begin therapeutic ultrasound treatments two to three times a week in an attempt to stop the calcium from congealing and halt the heel spur formation. We like to use the ultrasound combined with a technique I learned from an ancient Chinese doctor I spent time with many years ago. He taught me about a technique called “Gua Sha” and gave me his jade tool that he liked to use to perform it. When I began to use the Gua Sha tool to “scrape” the heel spur after the ultrasound treatment my results improved dramatically.
Surgery and other Treatments for Heel Spurs
I frequently get asked about surgery for heel spurs. Remember, it is not the spur that is painful. Rather, it is the FORMATION of the spur. Surgery to remove a heel spur can often result in complications and more pain and disability! Almost all patients can avoid surgery according the scientific research published in the National Library of Medicine.
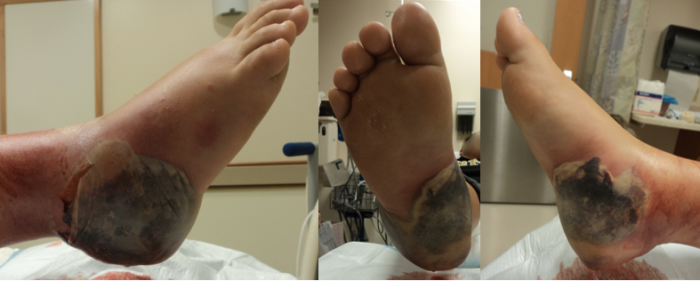
Botched surgery trying to fix a Heel Spur
Sometimes we do recommend a cortisone injection into the heel spur area but only if the person is resting and having the spur treated at that time. Cortisone is a powerful anti-inflammatory and can be used on occasion to help halt the spur formation. However, cortisone is also a powerful CATABOLIC hormone. A catabolic hormone is one that breaks things down….in this case your plantar fascia tendon is at risk due to its proximity to the heel spur. There have been quite a few studies that recommend against cortisone injections into this area because of the risk involved.
I also get asked about random treatments such as reflexology, acupuncture, lasers, prayer etc. While I do not deny that these treatments may be helpful for some I have not personally seen them be effective for the majority and do not recommend them for treating heel spurs.
If you have heel spurs and want help, an accurate diagnosis and effective treatment please let us help you. You can email me directly at [email protected] or you can call our clinic at 858-268-8525.