Metatarsalgia is a painful condition we frequently see at the San Diego Running Institute. This article will define “metatarsalgia” and provide possible causes and treatment options for metatarsal pain.
What is Metatarsalgia?
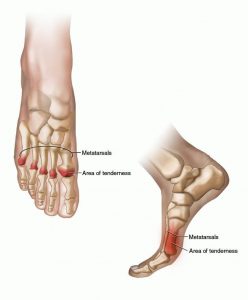
Metatarsalgia is a broad term used to describe pain the ball of the foot. The word “metatarsalgia” literally means “pain in the foot bones”. “Meta” means “metatarsal” (bones that make up your foot) and “algia” means pain. A metatarsalgia diagnosis can be frustrating, because you are usually already aware that you have foot pain!
Metatarsalgia Symptoms
A runner will complain of pain in the ball of their foot usually just behind the second or third toe. The pain can be intense or just a dull ache that they describe as “walking on a rock’ or “walking right on the bone”. Essentially the ligament that helps support and stabilize the 2-4th metatarsal bones and metatarsal arch is sprained. This causes laxity in the ligament which allow the metatarsal bones to “drop” and be lower to the ground. The pain can be intense enough to cause you to stop running.
Metatarsalgia is often misdiagnosed or confused with other common conditions, including:
- Plantar fasciitis
- Morton’s Neuroma
- Stress fractures
- Plantar plate sprain/tear
- Capsulitis
- Tendonitis
If you have pain in the ball of your foot or have been diagnosed with plantar fasciitis, Mortons Neuroma or metatarsalgia and have not been helped stop by the San Diego Running Institute and talk to one of our running specialists. You can also schedule an appointment with Dr. Allen by calling (858) 268-8525.
Metatarsalgia Diagnosis
It is important to know why you have metatarsalgia. There are many common conditions that can cause this type of foot pain. The San Diego Sports Injury Clinic employs techniques including:
- Manual orthopedic testing
- MRI for confirmation of diagnosis
- Instituting proper therapy as treatment
Metatarsalgia Treatment Options
Metatarsal pads are a common treatment option for metatarsalgia, but they must be applied correctly to be effective. Many runners and athletes have been to a foot doctor or sports doctor who made them custom sports orthotics with a metatarsal pad. When we ask the runner if it helps, they typically reply “No” and that “It does not help at all and may be making it worse”.
Using Metatarsal Pads
The problem is that the metatarsal pad has been placed incorrectly on the custom orthotic. It is essential to have the metatarsal pad in the correct location in order to ease the condition. As noted above, the ligament that helps support and stabilize the metatarsal bones and metatarsal arch is sprained. This allows the metatarsal bones to “drop” and be lower to the ground.
When the metatarsal pad is placed correctly just behind the metatarsal head (just behind the painful location) alleviation of the foot and arch pain is achieved. It is not unusual for us to correctly place a metatarsal pad for a patient and have them walk pain-free right then and there!
Properly placed metatarsal pads are a fast and effective treatment for metatarsalgia, but they are sometimes not enough to fix this common running foot injury. When this “quick-fix” fails the San Diego Running Institute can refer you to Dr. Bruce Allen. He is a foot pain specialist and has helped hundreds of runners and non-runners with metatarsalgia and other foot pain conditions.
Purchase Metatarsal Pads
Email: Info@sdri.net
Once you have them, do the following:
Step-by-Step Instructions for Placing Metatarsal Pads
- Take your insole out of your shoe and place it on the floor in front of you.
- While sitting, take a jar of liquid and place some with the applicator on the spot on your foot that is painful when you walk/run.
- Carefully place your foot on the insole and stand up while exerting a little pressure on the ball of your foot.
- Sit back down and remove your foot.
- Find the white mark on the insole, which is now representative of where your pain is.
- Remove 1/2 the backing on the metatarsal pad and stick it so that it is just behind your white mark.
- Put the insole back in the shoe and walk/run for a bit.
- You will “feel” where to move it there. You may have to move it millimeters to the right, left, front, or back to get the perfect spot but when you do, it should alleviate your pain/symptoms 50% – 100%
- After getting it in the perfect spot, take a Sharpie marker and trace the pad so the placement you will always know. Now remove the pad and take off the rest of the padding and stick it back down to the insole.
- Cover with Duct tape to prevent pad from coming off.
Please note the pad is not supposed to be beneath your pain. It is NOT a cushion for your painful area. It needs to be just BEHIND where your pain is, which is why the placement is so critical. Many patients have told me they tried metatarsal pads before and they did not work… they do work, they were just placed wrong.
Medical Journal Articles About Metatarsalgia & Related Conditions
[contentbox class=”contentbox3″]
Forefoot pain is one of the most common presenting problems in a foot and ankle practice. One of the most common presenting problems, yet most commonly missed problems, is a plantar plate tear. Often the problem is considered to be potential neuroma, fat pad atrophy, or a generalized diagnosis of metatarsalgia or metatarsal head overload. Unfortunately, not enough attention is placed on the plantar and medial/lateral ligamentous structures of the metatarsal-phalangeal joints. This lack of attention results in poor diagnosis, lack of care, treatment for the wrong condition, and ultimate frustration for the patients and doctor. “Plantar plate tears: a review of the modified flexor tendon transfer repair for stabilization.”– Originally Published by National Library of Medicine (NLM) in Jan, 2011.
[/contentbox]
[contentbox class=”contentbox2″]
OBJECTIVES:To determine the optimum position of a metatarsal (MT) pad to treat metatarsalgia. DESIGN:
We used a sensing mat with 16 x 16 sensors, 4.4 x 4.4 mm each, to measure plantar pressure in ten metatarsalgia patients walking with an MT pad in various positions. Peak pressures of the MT head and MT pad were analyzed. RESULTS:
Walking without MT pads, the peak pressure of the MT head was 678 +/- 227 and 687 +/- 228 kPa in one proximal and one distal row of three sensors. Placement of the MT pad resulting in peak pressure two sensors proximal to the peak pressure of the MT head did not significantly reduce peak pressure on the MT head. In contrast, placement of the MT pad resulting in peak pressure just proximal to the peak pressures of the MT head reduced the proximal and distal peak pressures on the MT head to 427 +/- 97 and 431 +/- 92 kPa (P < 0.05). CONCLUSIONS:
Optimum pressure reduction on the MT head is attained when the peak pressure generated by the MT pad is just proximal to the MT head. “Optimum position of metatarsal pad in metatarsalgia for pressure relief.” – Originally Published by National Library of Medicine (NLM) in July, 2005.
[/contentbox]
[contentbox class=”contentbox3″]
OBJECTIVE:The purpose of this study is to update a systematic review on manipulative therapy (MT) for lower extremity conditions. METHODS:
A review of literature was conducted using MEDLINE, MANTIS, Science Direct, Index to Chiropractic Literature, and PEDro from March 2008 to May 2011. Inclusion criteria required peripheral diagnosis and MT with or without adjunctive care. Clinical trials were assessed for quality using a modified Scottish Intercollegiate Guidelines Network (SIGN) ranking system. RESULTS:
In addition to the citations used in a 2009 systematic review, an additional 399 new citations were accessed: 175 citations in Medline, 30 citations in MANTIS, 98 through Science Direct, 54 from Index to Chiropractic Literature, and 42 from the PEDro database. Forty-eight clinical trials were assessed for quality. CONCLUSIONS:
Regarding MT for common lower extremity disorders, there is a level of B (fair evidence) for short-term and C (limited evidence) for long-term treatment of hip osteoarthritis. There is a level of B for short-term and C for long-term treatment of knee osteoarthritis, patellofemoral pain syndrome, and ankle inversion sprain. There is a level of B for short-term treatment of plantar fasciitis but C for short-term treatment of metatarsalgia and hallux limitus/rigidus and for loss of foot and/or ankle proprioception and balance. Finally, there is a level of I (insufficient evidence) for treatment of hallux abducto valgus. Further research is needed on MT as a treatment of lower extremity conditions, specifically larger trials with improved methodology. “Manipulative therapy for lower extremity conditions: update of a literature review.”
– Originally Published by National Library of Medicine (NLM) in Feb, 2012.
[/contentbox]
[contentbox class=”contentbox2″]
BACKGROUND:
Metatarsalgia is related to repetitive high-pressure loading under the metatarsal head (MH) that causes pain. The high pressure under the MH can be reduced by adequately applying metatarsal pads (MPs). Plantar pressure measurements may provide a method to objectively evaluate pressure loading under the MH. However, it is still unclear if the decrease in plantar pressure under the MH after MP treatment is associated with subjective improvement. This study aims to explore the correlations between subjective pain improvement and outcome rating, and the plantar pressure parameters in metatarsalgia patients treated using MPs.
METHODS:
Thirteen patients (a total of 18 feet) with secondary metatarsalgia were included in this study. Teardrop-shaped MPs made of polyurethane foam were applied just proximal to the second MH by an experienced physiatrist. Insole plantar pressure was measured under the second MH before and after MP application. Visual analog scale (VAS) scores of pain were obtained from all subjects before and after 2 weeks of MP treatment. The subjects rated using four-point subjective outcome scales. The Wilcoxon signed-rank test was used to analyze the difference between the plantar pressure parameters and VAS scores before and after treatment. The Kruskal-Wallis test was applied to compare the plantar pressure parameters in each outcome group. Pearson’s correlation was applied to analyze the correlation between the changes in plantar pressure parameters and VAS scores. Statistical significance was set as p < 0.05.
RESULTS:
MP application decreased the maximal peak pressure (MPP) and pressure-time integral (PTI) under the second MH and also statistically improved subjective pain scores. However, neither the pre-treatment values of the MPP and PTI shift in the position of the MPP after treatment, nor the age, gender and body mass index (BMI) of the subjects were statistically correlated with subjective improvement. Declines in the PTI and MPP values after MP application were statistically correlated with the improvement in VAS scores (r = 0.77, R2 = 0.59, p < 0.001; r = 0.60, R2 = 0.36, p = 0.009).
CONCLUSION:
We found that the successful decline in the PTI and MPP under the second MH after MP application was correlated to subjective pain improvement. This study provides a strategy for the further design and application of MPs for metatarsalgia treatment.
[/contentbox]
