Plantar Plate sprains (also known as Plantar Plate Tears) are common, painful conditions that can affect runners of all ages and experience levels.
What is a Plantar Plate Sprain?
A sprain is a torn ligament. Sprains occur in varying degrees of severity:
- Grade 1 Sprain describes a ligament that was overstretched which results in microtears and ligament laxity.
- Grade 2 Sprain is defined by partial tearing of the ligament resulting in more severe pain and possibly, partial joint deformity.
- Grade 3 Sprain is a complete tear of the ligament and results in intense pain with obvious joint deformity.
Since Plantar Plate Sprains come in varying degrees they are sometimes difficult for doctors who do not specialize in diagnosis and treatment of the disorder to identify and diagnose accurately.
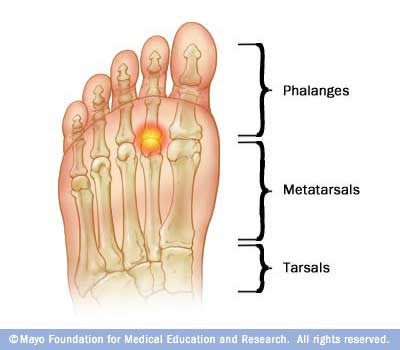
Plantar Plate Sprain Symptoms
Runners will typically describe intense pain near their 2nd through 4th toes in the ball of the foot that gets worse while walking or running. If you have pain beneath your 2nd, 3rd or 4th metatarsal, and it gets worse with walking, jumping or running, you may have a Plantar Plate Sprain. In the early stages of the injury it is most likely a Grade 1 Plantar Plate Sprain, which can be treated quickly and effectively using conservative methods. You will know if the injury has progressed if your pain gets worse or you develop a limp following activity.
Plantar Plate Sprain Diagnosis
Dr. Allen can perform a thorough orthopedic examination of your foot to accurately diagnose the condition and differentiate it from other conditions, such as:
- Morton’s Neuroma
- Metatarsal Stress Fracture
- Sesamoiditis
- Interdigital Bursitis
- Metatarsalgia
Differentiating these conditions is actually quite simple with proper manual, orthopedic testing. If there is still doubt after a thorough examination an MRI can be used to differentiate the disorders. San Diego Running Institute has brokered cash deals with private, local San Diego MRI facilities for those that have either no MRI coverage or catastrophic deductibles that often prevent them from obtaining proper care or treatment. The average cash fee for an MRI is only $500. X-rays can be performed the same day as the examination and do not require a scheduled appointment whereas an MRI can usually be performed within a couple of days.
Plantar Plate Sprain Treatment
The course of treatment depends on the severity of the tear. Grade 1 and Grade 2 Plantar Plate Sprains are treated with excellent outcomes at the San Diego Running Institute. Grade 3 Plantar Plate Sprains are more severe and will not typically respond to conservative treatment and may require surgery.
How To Fix A Sprained/Torn Plantar Plate Ligament
We never want to tell a runner to “Stop running”, but that is exactly what we have to do in most cases of a Plantar Plate Sprain. In mild cases we successfully treat the condition by placing Plantar Plate supports on the runner’s insoles of the shoes they wear most often. We also use waterproof athletic tape to align the joint to ensure maximum and effective healing. Therapeutic Ultrasound is applied to stimulate blood flow into the largely avasucular Plantar Plate Ligament. Simple exercises are prescribed to stimulate blood flow and promote strengthening of the deep intrinsic muscles of the foot.
Severe Grade 1 sprains and Grade 2 Plantar Plate Sprains usually require a stiff bottom walking boot for the runner to wear for six to twelve weeks depending on the severity of the sprain. This ensures that the patient is not flexing, bending or stretching the damaged Plantar Plate, and thus allows for complete, maximum healing. During the time period the patient is required to wear the boot there is a therapeutic protocol consisting of Ultrasound, taping and exercises that is also undertaken.
Surgery to Correct Torn Plantar Plate
Plantar plate surgery should only be considered if conservative treatment methods fail. It should be your last resort in most cases. We have found that 90% of patients treated with conservative methods do not require surgery, and they are able to return to normal, pain free running.
Torn Plantar Plate – Custom Orthotics
We often use custom orthotics to treat plantar plate pain, but they are not a perfect solution. The custom orthotic will most likely be ineffective if:
- The custom orthotic is not crafted correctly
- The plantar plate support is not placed precisely
- The injury is not addressed and given time to begin the healing process
It is our experience that after the injury is healed and the person resumes normal pain free activity a custom orthotic can be made to prevent future recurrences of the injury. San Diego Running Institute makes our own custom orthotics on site which helps keep the costs below average ($367) and gives us complete control in the construction of the orthotic. These are a great alternative to those made in orthotic labs; they often create hard, rigid orthotics that actually make the condition worse.
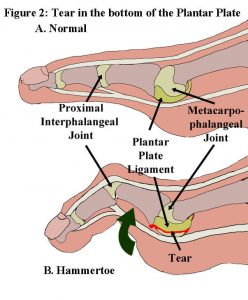
Healing Plantar Plate Sprains
If all of the correct procedures are followed there is no reason to expect anything less than 100% resolution of the condition.
Fibrin
By supporting and/or immobilizing the Plantar Plate, usually for a period of 6 weeks to 3 months, the ligament will heal by forming new tissue know as Fibrin. The new fibrotic tissue will essentially from a “patch” over the damaged area of the Plantar Plate. This new fibrotic tissue will at first be stiffer and may result in feelings of “tightness” beneath the Metatarsals.
Macrophages
Over the period of the next few months, even up to a year, the feelings of stiffness and tightness will lessen due to specialized cells in your body called Macrophages. These cells will reshape and reorganize the fibrotic tissue molding it as close to perfect as possible. It is our experience that making custom insoles with Plantar Plate supports provides additional protection to the area while it undergoes remodeling and strengthening and are a viable addition in the prevention of future recurrences.
Medical Journal Articles About Plantar Plate Pain
Forefoot pain is one of the most common presenting problems in a foot and ankle practice. One of the most common presenting problems, yet most commonly missed problems, is a plantar plate tear. Often the problem is considered to be potential neuroma, fat pad atrophy, or a generalized diagnosis of metatarsalgia or metatarsal head overload. Unfortunately, not enough attention is placed on the plantar and medial/lateral ligamentous structures of the metatarsal-phalangeal joints. This lack of attention results in poor diagnosis, lack of care, treatment for the wrong condition, and ultimate frustration for the patients and doctor. “Plantar plate tears: a review of the modified flexor tendon transfer repair for stabilization.”– Originally Published by National Library of Medicine (NLM) in Jan, 2011. OBJECTIVES:
To determine the optimum position of a metatarsal (MT) pad to treat metatarsalgia. DESIGN:
We used a sensing mat with 16 x 16 sensors, 4.4 x 4.4 mm each, to measure plantar pressure in ten metatarsalgia patients walking with an MT pad in various positions. Peak pressures of the MT head and MT pad were analyzed. RESULTS:
Walking without MT pads, the peak pressure of the MT head was 678 +/- 227 and 687 +/- 228 kPa in one proximal and one distal row of three sensors. Placement of the MT pad resulting in peak pressure two sensors proximal to the peak pressure of the MT head did not significantly reduce peak pressure on the MT head. In contrast, placement of the MT pad resulting in peak pressure just proximal to the peak pressures of the MT head reduced the proximal and distal peak pressures on the MT head to 427 +/- 97 and 431 +/- 92 kPa (P < 0.05). CONCLUSIONS:
Optimum pressure reduction on the MT head is attained when the peak pressure generated by the MT pad is just proximal to the MT head. “Optimum position of metatarsal pad in metatarsalgia for pressure relief.” – Originally Published by National Library of Medicine (NLM) in July, 2005. OBJECTIVE:
The purpose of this study is to update a systematic review on manipulative therapy (MT) for lower extremity conditions. METHODS:
A review of literature was conducted using MEDLINE, MANTIS, Science Direct, Index to Chiropractic Literature, and PEDro from March 2008 to May 2011. Inclusion criteria required peripheral diagnosis and MT with or without adjunctive care. Clinical trials were assessed for quality using a modified Scottish Intercollegiate Guidelines Network (SIGN) ranking system. RESULTS:
In addition to the citations used in a 2009 systematic review, an additional 399 new citations were accessed: 175 citations in Medline, 30 citations in MANTIS, 98 through Science Direct, 54 from Index to Chiropractic Literature, and 42 from the PEDro database. Forty-eight clinical trials were assessed for quality. CONCLUSIONS:
Regarding MT for common lower extremity disorders, there is a level of B (fair evidence) for short-term and C (limited evidence) for long-term treatment of hip osteoarthritis. There is a level of B for short-term and C for long-term treatment of knee osteoarthritis, patellofemoral pain syndrome, and ankle inversion sprain. There is a level of B for short-term treatment of plantar fasciitis but C for short-term treatment of metatarsalgia and hallux limitus/rigidus and for loss of foot and/or ankle proprioception and balance. Finally, there is a level of I (insufficient evidence) for treatment of hallux abducto valgus. Further research is needed on MT as a treatment of lower extremity conditions, specifically larger trials with improved methodology. “Manipulative therapy for lower extremity conditions: update of a literature review.”
– Originally Published by National Library of Medicine (NLM) in Feb, 2012.
BACKGROUND:
Metatarsalgia is related to repetitive high-pressure loading under the metatarsal head (MH) that causes pain. The high pressure under the MH can be reduced by adequately applying metatarsal pads (MPs). Plantar pressure measurements may provide a method to objectively evaluate pressure loading under the MH. However, it is still unclear if the decrease in plantar pressure under the MH after MP treatment is associated with subjective improvement. This study aims to explore the correlations between subjective pain improvement and outcome rating, and the plantar pressure parameters in metatarsalgia patients treated using MPs.
METHODS:
Thirteen patients (a total of 18 feet) with secondary metatarsalgia were included in this study. Teardrop-shaped MPs made of polyurethane foam were applied just proximal to the second MH by an experienced physiatrist. Insole plantar pressure was measured under the second MH before and after MP application. Visual analog scale (VAS) scores of pain were obtained from all subjects before and after 2 weeks of MP treatment. The subjects rated using four-point subjective outcome scales. The Wilcoxon signed-rank test was used to analyze the difference between the plantar pressure parameters and VAS scores before and after treatment. The Kruskal-Wallis test was applied to compare the plantar pressure parameters in each outcome group. Pearson’s correlation was applied to analyze the correlation between the changes in plantar pressure parameters and VAS scores. Statistical significance was set as p < 0.05.
RESULTS:
MP application decreased the maximal peak pressure (MPP) and pressure-time integral (PTI) under the second MH and also statistically improved subjective pain scores. However, neither the pre-treatment values of the MPP and PTI shift in the position of the MPP after treatment, nor the age, gender and body mass index (BMI) of the subjects were statistically correlated with subjective improvement. Declines in the PTI and MPP values after MP application were statistically correlated with the improvement in VAS scores (r = 0.77, R2 = 0.59, p < 0.001; r = 0.60, R2 = 0.36, p = 0.009).
CONCLUSION:
We found that the successful decline in the PTI and MPP under the second MH after MP application was correlated to subjective pain improvement. This study provides a strategy for the further design and application of MPs for metatarsalgia treatment.
